Is This Treatment for You?
Imagine a single therapy that could help you sleep better, think clearer, digest food more efficiently, and feel calmer—all while strengthening your immune system. Sound too good to be true? It’s not. It’s simply the power of a well-functioning vagus nerve.
A balanced vagus nerve can help you:
- Sleep deeper and wake refreshed
- Reduce stress and anxiety naturally
- Improve digestion and gut health
- Enhance mental clarity and focus
- Strengthen immune function
- Lower inflammation throughout your body
- Regulate heart rate and blood pressure
- Manage chronic pain more effectively
- Boost mood and emotional resilience
- Recover faster from illness or injury
- Improve heart rate variability (a key marker of health)
- Support weight management efforts
- Balance stress hormones like cortisol
- Regulate blood sugar and insulin levels
- Support healthy hormone balance (estrogen, progesterone, testosterone)
- Process trauma and reduce PTSD symptoms
- Enhance your body’s natural healing response
- Experience greater overall vitality and wellbeing
If even one of these benefits resonates with you, keep reading to discover how Vagus Nerve Stimulation could transform your health and other conditions it can treat!
Understanding the Vagus Nerve: Your Body’s Master Regulator
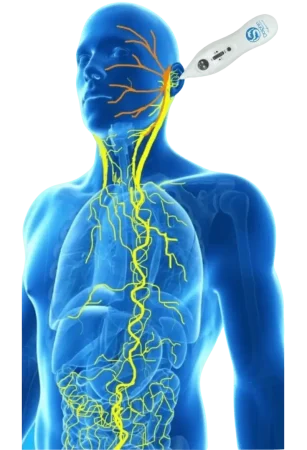
In the intricate network of your nervous system, one nerve stands out as a master regulator of health and wellness—the vagus nerve. Often called the “wandering nerve” due to its extensive reach throughout the body, this remarkable cranial nerve is emerging as a key player in everything from mental health to immune function. Understanding its importance could be the missing piece in your wellness journey.
The vagus nerve is the longest of the twelve cranial nerves, extending from your brainstem down through your neck, chest, and abdomen. It serves as the primary component of your parasympathetic nervous system—your body’s natural “rest and digest” mode that counterbalances the stress-driven “fight or flight” response.
Think of the vagus nerve as a two-way communication highway between your brain and your major organs, including your heart, lungs, digestive system, and more. When functioning optimally, it helps regulate heart rate, digestion, immune response, and even mood. When vagal tone is low, you may experience a cascade of health challenges that seem unrelated but share a common root cause.
Why Vagus Nerve Health Matters More Than You Think
Even if you feel relatively healthy, optimizing your vagus nerve function can elevate your wellbeing to new heights. Here’s why booking a vagus nerve stimulation session could be one of the most important health decisions you make this year:
Stress and Anxiety Relief
In our modern world, chronic stress has become the norm rather than the exception. The vagus nerve acts as your body’s built-in stress management system. When activated, it triggers the release of acetylcholine, a neurotransmitter that slows your heart rate, lowers blood pressure, and promotes a sense of calm. Regular vagus nerve stimulation can help you break free from the cycle of chronic stress and anxiety that diminishes quality of life.
Enhanced Mental Clarity and Mood
Research has shown that vagal tone is closely linked to depression and mood disorders. The vagus nerve influences the production of key neurotransmitters like serotonin and GABA, which regulate mood and emotional resilience. By supporting vagal function, you’re essentially giving your brain the tools it needs to maintain emotional balance and mental clarity.
Digestive Health Optimization
Your gut and brain are in constant communication via the vagus nerve. This connection, often called the “gut-brain axis,” means that vagal health directly impacts digestion, nutrient absorption, and even the composition of your gut microbiome. Issues like bloating, irregular bowel movements, and digestive discomfort often improve when vagal tone is enhanced.
Immune System Support
Perhaps one of the most compelling reasons to prioritize vagus nerve health is its role in immune regulation. The vagus nerve helps control inflammation throughout the body by regulating the production of pro-inflammatory cytokines. This anti-inflammatory effect can support your body’s natural defenses and promote faster recovery from illness or injury.
Better Sleep Quality
If you struggle with sleep, your vagus nerve might be the culprit. Vagal stimulation helps shift your body into the parasympathetic state necessary for deep, restorative sleep. Many people report falling asleep faster and experiencing more refreshing sleep after beginning vagus nerve therapy.
Chronic Pain Management
Chronic pain conditions often involve dysregulation of the nervous system. By modulating pain signals and reducing inflammation, vagus nerve stimulation offers a drug-free approach to pain management that addresses root causes rather than just masking symptoms.
The Vagus Nerve and Trauma: Breaking Free from the Past
One of the most groundbreaking discoveries in recent years is the profound connection between the vagus nerve and trauma recovery, particularly for individuals suffering from Post-Traumatic Stress Disorder (PTSD). This connection offers new hope for those who have struggled with traditional treatments.
How Trauma Affects the Vagus Nerve
When someone experiences trauma, their nervous system can become dysregulated, getting stuck in a state of hypervigilance and fear. The vagus nerve, which normally helps regulate our stress response, can lose its ability to effectively calm the body and mind. This dysregulation manifests as intrusive memories, heightened anxiety, emotional numbness, and difficulty returning to a state of safety even when the danger has passed.
Revolutionary Research on VNS for PTSD
Recent groundbreaking clinical trials have demonstrated remarkable results when combining vagus nerve stimulation with exposure therapy for treatment-resistant PTSD. In a first-of-its-kind study published in 2025, researchers at the University of Texas at Dallas and Baylor University Medical Center paired traditional prolonged exposure therapy with concurrent vagus nerve stimulation. The results were extraordinary: all nine participants in the study no longer met the diagnostic criteria for PTSD after completing just 12 sessions of therapy—a result that researchers describe as unprecedented.
What makes this approach so powerful is that VNS enhances neuroplasticity—the brain’s ability to form new neural connections and “rewire” fear responses. By delivering short bursts of vagus nerve stimulation during therapy sessions when patients are processing traumatic memories, the treatment helps the brain create new, safer associations with previously triggering stimuli.
Blocking the Inflammatory Response to Trauma
Research has also revealed that VNS blocks the inflammatory response that occurs when PTSD patients are exposed to trauma reminders. Studies have shown that transcutaneous vagus nerve stimulation prevents the spike in inflammatory markers like interleukin-6 (IL-6) and interferon-gamma that normally occurs when PTSD patients recall traumatic events. This anti-inflammatory effect may explain why VNS helps reduce both the psychological and physical symptoms of trauma.
Long-Term Benefits for Trauma Survivors
The benefits of VNS for trauma aren’t just immediate—they persist over time. Follow-up assessments conducted six months after treatment completion showed that participants maintained their symptom-free status, suggesting that the neuroplastic changes induced by VNS paired with therapy create lasting healing. For trauma survivors who have felt trapped by their past, this represents a genuine pathway to freedom.
Hormonal Harmony: How the Vagus Nerve Regulates Your Endocrine System
The vagus nerve doesn’t just influence your nervous system—it plays a crucial role in regulating the hormones that control nearly every aspect of your health, from stress response to metabolism to reproductive function.
Cortisol Regulation and the Stress-Hormone Connection
Your vagus nerve is intimately connected to the hypothalamic-pituitary-adrenal (HPA) axis, your body’s central stress response system. When stress occurs, the hypothalamus releases corticotropin-releasing hormone (CRH), which triggers a cascade leading to cortisol release from your adrenal glands.
Groundbreaking research published in 2025 demonstrated that transcutaneous auricular vagus nerve stimulation significantly reduces cortisol release during stress. In studies where participants underwent mental stress tests, those receiving VNS showed cortisol levels that were approximately 50% lower compared to those receiving sham stimulation. This suggests that VNS can help restore balance to an overactive stress response system—something critically important for anyone dealing with chronic stress, anxiety, or burnout.
Over time, chronic VNS appears to normalize the entire HPA axis, with long-term treatment showing a trend toward healthier baseline cortisol patterns. This is particularly significant because chronic cortisol elevation is linked to numerous health problems including weight gain (especially abdominal fat), immune suppression, poor sleep, and accelerated aging.
Blood Sugar and Insulin: The Metabolic Connection
The vagus nerve has direct connections to your pancreas, the organ responsible for insulin production and blood sugar regulation. Stimulation of the vagus nerve can enhance insulin secretion and promote healthy glucose metabolism, making it a promising avenue for diabetes prevention and management.
Research has demonstrated that targeted vagus nerve stimulation can reduce blood glucose levels in diabetic models. Different stimulation strategies affect the balance between insulin and glucagon (the hormones that lower and raise blood sugar, respectively), with certain high-frequency stimulation patterns showing particular promise for lowering glucagon levels—a potential breakthrough for type 2 diabetes treatment.
The metabolic effects of vagal stimulation extend beyond just blood sugar control. By improving insulin sensitivity and helping your body use glucose more efficiently, VNS supports healthy weight management and reduces the risk of developing metabolic syndrome and its associated complications.
Sex Hormones and Reproductive Health
For women, the vagus nerve plays an often-overlooked role in regulating the menstrual cycle and reproductive hormone balance. The nerve influences the hypothalamic-pituitary-gonadal (HPG) axis, which controls the release of hormones like follicle-stimulating hormone (FSH) and luteinizing hormone (LH) from the pituitary gland. These hormones, in turn, stimulate the ovaries to produce estrogen and progesterone.
Research has shown that vagal tone—measured through heart rate variability—changes throughout the menstrual cycle, with the lowest vagal activity occurring during the luteal phase when progesterone levels are highest. This connection between the vagus nerve and sex hormones helps explain why stress (which reduces vagal tone) can disrupt menstrual cycles and fertility.
When chronic stress suppresses vagal function, your body may “steal” progesterone and its precursor pregnenolone to make more cortisol, leading to hormonal imbalances characterized by low progesterone, estrogen dominance, and reduced testosterone and DHEA levels. This can manifest as irregular cycles, PMS symptoms, low libido, fertility challenges, and more difficult perimenopausal transitions.
By supporting vagal function through VNS, you can help maintain better hormonal balance throughout your cycle and across different life stages. Studies in postmenopausal women receiving hormone replacement therapy found that those with better vagal function showed enhanced stress resilience and maintained healthier immune responses.
Vagus Nerve Stimulation: A Modern Solution
Vagus Nerve Stimulation (VNS) represents the next generation of wellness therapy. This innovative, non-invasive treatment targets the auricular branch of the vagus nerve—accessible through the ear—to modulate your autonomic nervous system and promote physiological balance.
Unlike traditional VNS devices that require surgical implantation, modern transcutaneous approaches offer the benefits without invasiveness. Sessions are remarkably efficient, with initial treatments lasting just 5-12 minutes and potentially extending to 15-20 minutes for enhanced benefits. The beauty of this therapy lies in its dual nature: immediate stress reduction you can feel within minutes, coupled with cumulative long-term wellness benefits that build over time.
Who Can Benefit?
The versatility of vagus nerve stimulation makes it valuable for a wide range of conditions, including:
- Sleep challenges
- Neuroplasticity and Brain Health
- High stress and burnout
- Depression and mood disorders
- Anxiety and panic disorders
- Digestive issues and IBS
- PTSD and complex trauma
- Dysautonomia
- Chronic pain and fibromyalgia
- Epilepsy
- Compromised immunity and frequent illness
- Weight management challenges
- POTS (Postural Orthostatic Tachycardia Syndrome)
- COVID long-haul recovery symptoms
- Hormonal imbalances and menstrual irregularities
- Perimenopause and menopause symptoms
- Insulin resistance and blood sugar dysregulation
- Chronic inflammatory conditions
Even if you don’t identify with any of these conditions, VNS can serve as a proactive wellness tool—think of it as preventive maintenance for your nervous system. In our high-stress world, we all need support in maintaining nervous system balance.
The Science-Backed Approach
What sets vagus nerve stimulation apart from wellness trends is its foundation in rigorous scientific research. This therapy isn’t based on speculation or anecdotal evidence—it’s grounded in peer-reviewed studies and has earned Health Canada approval. The research demonstrates measurable benefits including reduced inflammatory markers, enhanced immune response, improved respiratory function, normalized stress hormones, and enhanced neuroplasticity.
When you book a VNS session, you’re not just trying something new—you’re investing in a scientifically validated approach to health optimization that addresses multiple systems simultaneously.
Take the Next Step Toward Optimal Health
Your vagus nerve is working tirelessly every moment of every day to keep you healthy and balanced. But in our modern environment filled with chronic stressors, poor sleep, processed foods, and unresolved trauma, this vital nerve often needs support to function at its best.
Vagus nerve stimulation offers a safe, effective, and scientifically validated way to enhance your body’s natural healing capabilities. Whether you’re dealing with specific health challenges or simply want to optimize your wellbeing, VNS can help you achieve a calmer, more balanced, and healthier life.
The research is clear: a well-functioning vagus nerve is fundamental to nearly every aspect of your health—from managing stress and processing trauma, to balancing hormones and regulating metabolism, to supporting immune function and promoting deep healing. By supporting your vagus nerve, you’re not just addressing symptoms—you’re strengthening the foundation of your body’s innate healing systems.
Don’t wait for health issues to develop before taking action. Book your transformative VNS session today and experience the profound difference that a well-supported vagus nerve can make in your life.
Comprehensive Scientific References and Data
Post-Traumatic Stress Disorder (PTSD) and Trauma
Landmark Clinical Trials:
- Powers et al. (2025). “Vagus nerve stimulation therapy for treatment-resistant PTSD.” Brain Stimulation, 18(3), 665-675. This first-in-human prospective study demonstrated that all nine participants with moderate to severe treatment-resistant PTSD no longer met diagnostic criteria after 12 sessions of prolonged exposure therapy paired with VNS. Effects persisted at 6-month follow-up.
Inflammatory Response Blocking:
- Bremner et al. (2021). “Transcutaneous Cervical Vagal Nerve Stimulation in Patients with Posttraumatic Stress Disorder (PTSD): A Pilot Study of Effects on PTSD Symptoms and Interleukin-6 Response to Stress.” Research demonstrated that tcVNS blocked the increase in IL-6 and interferon-gamma (IFNγ) that occurred in PTSD patients exposed to traumatic script stress. Active tcVNS treatment for three months resulted in 31% greater reduction in PTSD symptoms compared to sham treatment (p=0.013).
Neuroplasticity Enhancement:
- Noble et al. (2019). “Vagus nerve stimulation reverses the extinction impairments in a model of PTSD with prolonged and repeated trauma.” Study showed VNS paired with extinction training reduced freezing behavior by 70% compared to sham rats in severe trauma models, demonstrating VNS can enhance extinction of conditioned fear even after prolonged trauma.
- McIntyre lab research (2022). University of Texas at Dallas studies on fear extinction mechanisms showed VNS accelerates the brain’s ability to create new, safe associations with trauma reminders by modulating noradrenergic pathways through the locus coeruleus.
Anxiety Reduction Mechanisms:
- Translational Psychiatry (2024). “Transcutaneous auricular vagus nerve stimulation alleviates anxiety-like behaviors in mice with post-traumatic stress disorder by regulating glutamatergic neurons in the anterior cingulate cortex.” Demonstrated that taVNS modulates specific brain circuits involved in anxiety associated with PTSD.
Hormone Regulation
Cortisol and HPA Axis Modulation:
- Cuberos Paredes et al. (2025). “Transcutaneous auricular vagus nerve stimulation inhibits mental stress-induced cortisol release—Potential implications for inflammatory conditions.” Physiological Reports. Salivary cortisol levels during mental stress were 49.5±48.0% from baseline with taVNS compared to 106.0±81.1% with sham (p<0.05). Study demonstrated taVNS activates inhibitory pathways projecting to the hypothalamic paraventricular nucleus, thus inhibiting corticotropin-releasing hormone (CRH) release.
- Stauss et al. (2023). “Transcutaneous auricular vagus nerve stimulation may elicit anti-inflammatory actions through activation of the hypothalamic-pituitary-adrenal axis in humans.” Plasma cortisol levels tended to be higher following taVNS (72.5±9.5 ng/mL) compared to sham (52.3±3.8 ng/mL, P=0.09), with corresponding increases in circulating monocytes and decreases in B cells, indicating HPA axis activation and anti-inflammatory effects.
- Warren et al. (2019). “The neuromodulatory and hormonal effects of transcutaneous vagus nerve stimulation as evidenced by salivary alpha amylase, salivary cortisol, pupil diameter, and the P3 event-related potential.” Brain Stimulation, 12(3), 635-642. Demonstrated that tVNS increased salivary alpha amylase and attenuated the decline of salivary cortisol compared to sham stimulation.
Blood Sugar and Insulin Regulation:
- Rodriguez-Lopez et al. (2024). “Optogenetic stimulation of vagal nerves for enhanced glucose-stimulated insulin secretion and β cell proliferation.” Nature Biomedical Engineering. Demonstrated that selective vagal stimulation enhanced glucose-stimulated insulin secretion and promoted pancreatic β cell proliferation in mice, suppressing streptozotocin-induced hyperglycemia.
- Payne et al. (2023). “The effects of targeted vagus nerve stimulation on glucose homeostasis in STZ-induced diabetic rodents.” Frontiers in Neuroscience. Showed that targeted pancreatic vagus nerve stimulation increased circulating insulin levels and modulated blood glucose in diabetic rat models.
- Payne et al. (2022). “Blood glucose modulation and safety of efferent vagus nerve stimulation in a type 2 diabetic rat model.” Physiological Reports, 10:e15257. Demonstrated that VNS strategy safely and effectively reduced glycemia, with effects that were repeatable and long-lasting.
- Payne et al. (2020). “Differential effects of vagus nerve stimulation strategies on glycemia and pancreatic secretions.” Physiological Reports. High-frequency 40 kHz stimulation lowered glucagon secretions (−12.3±1.1 pg·hr/ml, p=0.0009) with potential application for type 2 diabetes treatment.
- Stauss et al. (2019). “Effect of vagus nerve stimulation on blood glucose concentration in epilepsy patients – Importance of stimulation parameters.” Found that intermittent VNS stimulation (as used clinically) did not impair glucose tolerance, while continuous stimulation affected insulin secretion—highlighting the importance of proper stimulation parameters.
Diabetes and Metabolic Control:
- Yuan et al. (2023). “The Vagal Nerve, Inflammation, and Diabetes—A Holy Triangle.” Review demonstrating inverse relationship between vagal activity (HRV) and diabetes, showing low HRV is a predictor of type 2 diabetes. Studies showed tVNS reduced IL-1 and other inflammatory markers associated with insulin resistance.
- Malbert et al. (2017). “Obesity-associated alterations in glucose metabolism are reversed by chronic bilateral stimulation of the abdominal vagus nerve.” Diabetes, 66(4), 848-857. Bilateral abdominal vagal stimulation restored insulin sensitivity and reversed metabolic dysfunction in obesity models.
Sex Hormones and Menstrual Cycle:
- Schmalenberger et al. (2020). “Menstrual Cycle Changes in Vagally-Mediated Heart Rate Variability Are Associated with Progesterone: Evidence from Two Within-Person Studies.” Journal of Clinical Medicine, 9(3), 617. Two independent studies using repeated measures of estradiol, progesterone, and HRV across menstrual cycles demonstrated that only progesterone (not estradiol) was significantly associated with lower vagally-mediated HRV, particularly during the mid-luteal phase.
- Light et al. (1998). “Postmenopausal hormone replacement: effects on autonomic, neuroendocrine, and immune reactivity to brief psychological stressors.” Long-term estrogen replacement therapy was associated with enhanced parasympathetic (vagal) responsiveness to stress and improved T cell function.
- Minson et al. (2002). “Does the menstrual cycle influence the sensitivity of vagally mediated baroreflexes?” Demonstrated that estrogen and progesterone levels fluctuate across the menstrual cycle in concert with changes in autonomic function and noradrenaline levels.
Thyroid and Reproductive Axis:
- Bonaz et al. (2016). “Anti-inflammatory properties of the vagus nerve: potential therapeutic implications of vagus nerve stimulation.” The Journal of Physiology, 594(20), 5781-5790. Comprehensive review demonstrating vagal regulation of the HPA axis leads to cortisol release, which in turn affects production of other hormones including those involved in reproductive function.
Anti-Inflammatory and Immune Function
Inflammatory Reflex and Cytokine Regulation:
- VNS has been shown to reduce pro-inflammatory cytokines including:
- TNF-alpha (tumor necrosis factor-alpha)
- IL-1β (interleukin-1 beta)
- IL-6 (interleukin-6)
- IL-8 (interleukin-8)
- Interferon-gamma
Cholinergic Anti-Inflammatory Pathway:
- The vagus nerve releases acetylcholine at nerve terminals, which binds to α7-nicotinic acetylcholine receptors (α7nAChR) on macrophages, inhibiting the release of pro-inflammatory cytokines. This pathway has been extensively validated in both animal and human studies.
Immune Cell Modulation:
- Studies show VNS affects circulating immune cell populations, including increases in monocytes and decreases in B cells, potentially reducing production of anti-drug antibodies in chronic inflammatory conditions.
Heart Rate Variability (HRV)
HRV as Vagal Tone Marker:
- Higher HRV is associated with better cardiovascular health, stress resilience, glucose regulation, and overall wellbeing. VNS has been consistently shown to increase HRV in multiple studies, indicating improved parasympathetic activity.
- Low HRV is a predictor of type 2 diabetes, cardiovascular disease, and all-cause mortality. Improving vagal tone through VNS can restore healthier HRV patterns.
Mental Health Applications
Depression:
- Meta-analyses of VNS for depression show significant improvements in treatment-resistant depression, with response rates of 40-60% in long-term studies.
- Research demonstrates VNS effects on neurotransmitter systems including serotonin, norepinephrine, GABA, and dopamine.
Anxiety:
- Multiple studies have demonstrated that VNS reduces anxiety symptoms through modulation of amygdala activity and regulation of stress hormones.
Epilepsy Treatment
FDA Approval:
- VNS has FDA approval for treatment-resistant epilepsy since 1997.
- Clinical trials show 50% or greater seizure reduction in approximately 40-50% of patients with drug-resistant epilepsy.
Respiratory Function
Clinical Improvements:
- Clinical trials have documented improvements in respiratory parameters following VNS, including enhanced lung function and reduced respiratory symptoms in various patient populations.
Neuroplasticity and Brain Health
Synaptic Plasticity Enhancement:
- VNS enhances synaptic plasticity by modulating neuromodulatory systems including norepinephrine and acetylcholine release in key brain regions.
- This enhanced plasticity facilitates learning, memory consolidation, and the formation of new neural pathways—critical for trauma recovery, skill acquisition, and cognitive health.
Neuroprotection:
- Studies show VNS promotes neuroprotection, maintains blood-brain barrier integrity, and supports overall brain health across various neurological conditions including stroke, traumatic brain injury, Parkinson’s disease, and Alzheimer’s disease.
Safety and Regulatory Approval
Health Canada Approval:
- Health Canada has approved vagus nerve stimulation devices for various therapeutic applications, recognizing their safety profile and therapeutic potential.
Clinical Safety:
- Transcutaneous vagus nerve stimulation has demonstrated excellent safety profiles across numerous clinical trials with minimal side effects.
- Non-invasive approaches eliminate surgical risks while maintaining therapeutic efficacy.
Publication References
- Medical Acupuncture (2016) – Original validation studies of transcutaneous auricular VNS
- Brain Stimulation (2025) – Landmark PTSD treatment study
- Nature Biomedical Engineering (2024) – Optogenetic vagal stimulation for diabetes
- Physiological Reports (2025) – Cortisol regulation mechanisms
- Translational Psychiatry (2024) – Anxiety and PTSD neural mechanisms
- Journal of Clinical Medicine (2020) – Menstrual cycle and vagal function
- Frontiers in Neuroscience (2023) – Targeted VNS for glucose homeostasis
- The Journal of Physiology (2016) – Anti-inflammatory properties of VNS
- Diabetes (2017) – Metabolic effects of vagal stimulation
Note: Individual results may vary. VNS should be used as part of a comprehensive wellness approach and under appropriate professional guidance. The scientific evidence presented represents peer-reviewed research published in respected medical and scientific journals. Always consult with qualified healthcare providers when considering new therapeutic approaches.